Getting the right dose of liquid medicine isn’t just about following the label-it’s about understanding exactly what it says. A wrong measurement can mean the difference between healing and harm. In the U.S., an estimated 1.3 million injuries each year come from medication errors, and nearly half of those involve liquid prescriptions for kids. The good news? The system has changed. Most pharmacies now use a single, clear standard: milliliters (mL). But if you’ve ever stared at a label wondering if 5 mL is the same as a spoonful, you’re not alone. Here’s how to read it right.
What’s on the label? Three key pieces
Every liquid prescription label has three critical parts you need to check every time:
- Total container volume - This tells you how much liquid is in the bottle. It’s usually printed near the bottom and looks like "120 mL" or "240 mL." This is NOT the dose. It’s just how much medicine the bottle holds.
- Concentration - This is the most important number. It tells you how much medicine is in each milliliter. It’s written like: "160 mg / 5 mL" or "125 mg per 5 mL." That means every 5 mL of liquid contains 160 mg (or 125 mg) of the active drug.
- Dosage instructions - This says how much to give and how often. It might say: "Take 10 mL every 6 hours." Or, "Give 2.5 mL once daily." Always match this number to the concentration to find the right amount.
Here’s a real example: Your child’s prescription says:
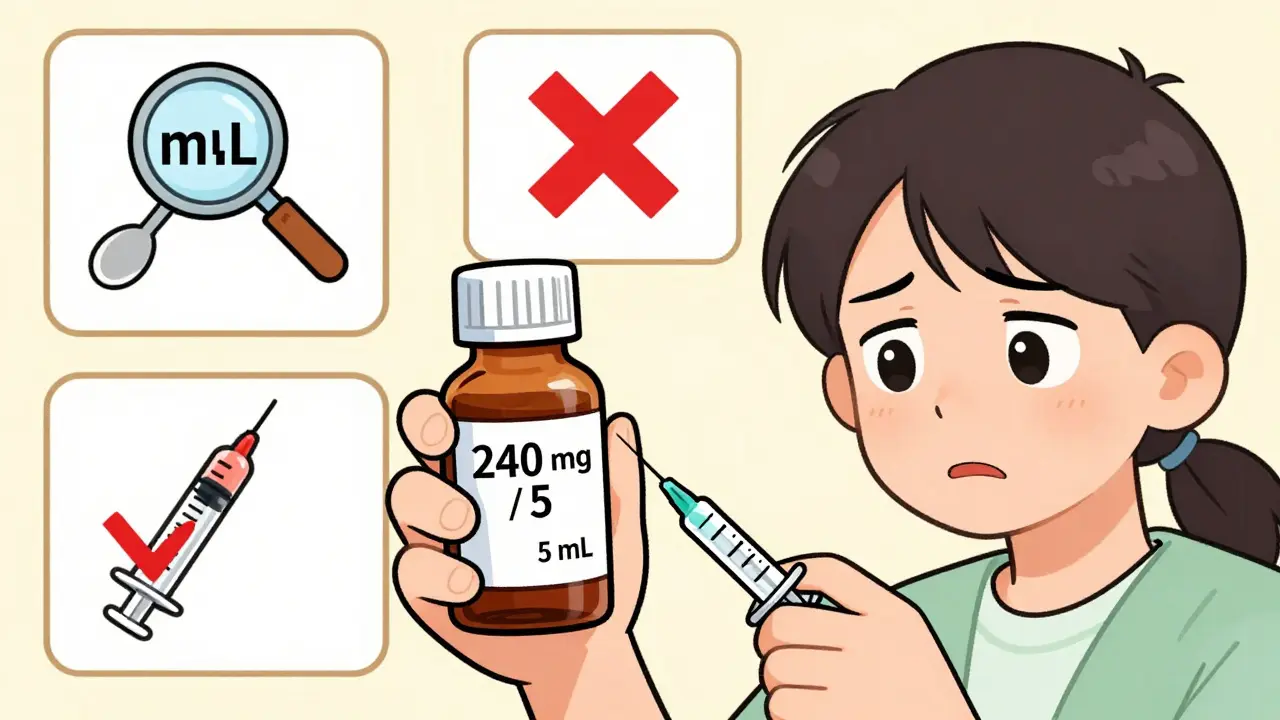
- Concentration: 240 mg / 5 mL
- Dosage: Give 120 mg every 8 hours
That means you don’t give 120 mg straight. You give the amount of liquid that contains 120 mg. Since 5 mL contains 240 mg, half of that (2.5 mL) contains 120 mg. So you give 2.5 mL-not 120 mL. Mixing up the number on the label with the dose is one of the most common mistakes.
Why milliliters (mL) and not teaspoons?
Older labels used to say "1 tsp" or "1 tbsp." That’s gone. Why? Because a teaspoon isn’t a teaspoon. A household spoon can hold anywhere from 2.5 mL to 7.5 mL. A tablespoon? It can be 5 mL or 20 mL. That’s a 300% difference. A 2016 study in the Journal of Pediatrics found parents using spoons were twice as likely to give the wrong dose compared to those using mL-measured devices.
The National Council for Prescription Drug Programs (NCPDP) and the FDA now require all liquid prescriptions to use only milliliters. This isn’t optional. By 2020, 92% of major pharmacy chains like CVS and Walgreens had switched. Even independent pharmacies are catching up-though not all are there yet.
And here’s a small but life-saving detail: numbers on the label must be written a certain way. If the dose is less than 1 mL, it must start with a zero. So it says 0.5 mL, not .5 mL. If it’s 5 mL, it must not say 5.0 mL. That trailing zero used to cause confusion-someone might read 5.0 as 50. Johns Hopkins found this simple rule cut 10-fold dosing errors by 47%.
What about the measuring device?
The bottle might come with a plastic cup or syringe. That’s your tool. Never use a kitchen spoon-not even if it says "teaspoon" on it. The measuring device should match the label’s units. If the label says mL, the cup or syringe should have mL markings.
Check the markings. Some devices go up to 0.1 mL. Others only show every 1 mL. If your dose is 3.7 mL and your syringe only has marks at 3 mL and 4 mL, you’re stuck. That’s why some pharmacies now include syringes with finer lines. Always ask for one if you’re unsure.
And here’s something most people don’t realize: the measuring device might not be accurate. A 2016 study found that over-the-counter dosing cups had a 98.6% mismatch between what they showed and what they actually held. That’s why you should use the one that came with the prescription-not a leftover from last time.

What if the label is confusing?
You’re not supposed to guess. If you see something like:
- "240 mg / 5 mL" and the dose says "Take 1 mL"
- "500 mL" on the bottle and you think that’s the dose
- ".8 mL" and you’re not sure if that’s 8 mL
Stop. Call the pharmacy. Ask: "Can you walk me through this?" Pharmacists are trained to explain this. They should have given you a demonstration when you picked it up. If they didn’t, ask now. Don’t wait until you’re at home with a crying child.
A 2021 study from Memorial Sloan Kettering found that patients who repeated back the instructions-known as the "teach-back" method-made 63% fewer mistakes. Try saying it out loud: "So, the medicine is 160 mg in every 5 mL, and I need to give 80 mg. That means I give half of 5 mL, which is 2.5 mL. Got it." If you can say it clearly, you probably got it right.
What about children and infants?
Most liquid medicines are for kids. About 75% of all liquid prescriptions are for children under 12. And the doses? Tiny. Sometimes as small as 0.8 mL for a baby. That’s less than two drops. This is why precision matters so much.
Infant doses are often written in decimals: 0.4 mL, 0.7 mL. No rounding. If the label says 0.7 mL, you give exactly 0.7 mL. Use a syringe. Never pour from a cup. Syringes are the most accurate tool for these small amounts. Most pharmacies will give you one for free if you ask.
And don’t assume a "children’s" label is safe. Some children’s acetaminophen is 160 mg/5 mL. Others are 100 mg/5 mL. If you switch brands, the dose changes. Always check the concentration.

What’s changing in 2026?
Things are getting even clearer. In 2023, the FDA proposed new rules requiring pictograms on all liquid medicine labels-simple pictures showing how to fill a syringe or cup. A 2022 study showed visual aids cut errors by 37%. By 2026, you’ll likely see a little drawing next to the dose: a syringe with a line at 5 mL, or a cup with an arrow pointing to the right level.
Some pharmacies are already testing QR codes. Scan it, and a short video plays showing exactly how to measure the dose. Amazon Pharmacy and McKesson’s Medly system are leading this. It’s not everywhere yet-but it’s coming.
Also, by 2025, Medicare will start penalizing pharmacies that don’t follow the mL-only standard. That means even small, independent pharmacies will have to upgrade their systems. The goal? Zero errors. The path? Clear labels, proper tools, and patient education.
What to do next
When you get a liquid prescription:
- Look for the concentration: "___ mg / ___ mL"
- Find the dose: "Take ___ mL"
- Use the measuring device that came with it-never a spoon
- If you’re unsure, call the pharmacy and ask them to explain it out loud
- Ask for a syringe if the dose is under 5 mL
And if you’ve ever given the wrong dose? You’re not alone. But now you know how to avoid it. The system is designed to protect you. You just have to read it right.
Can I use a kitchen teaspoon if I don’t have a measuring cup?
No. A kitchen teaspoon can hold anywhere from 2.5 mL to 7.5 mL. That’s a huge difference. If your child’s dose is 5 mL, using a spoon might mean giving 7 mL-almost 40% too much. Always use the measuring device that came with the medicine. If you lost it, call the pharmacy. They’ll give you a new one for free.
Why does the label say "160 mg/5 mL"? Isn’t that confusing?
It looks confusing at first, but it’s actually the clearest way. The "160 mg" is the amount of active medicine. The "5 mL" is the volume of liquid it’s mixed in. So if you need 80 mg, you give half of 5 mL, which is 2.5 mL. This system lets pharmacies make one bottle that can be used for different doses-instead of having a separate bottle for every strength.
What if the dose is 0.8 mL? How do I measure that?
Use a 1 mL oral syringe. These are designed for exact small doses. Most pharmacies will give you one at no cost. Don’t try to estimate with a cup. Even a 0.1 mL error can matter in babies. A syringe lets you pull back to the exact line. If you’re not sure how to use it, ask the pharmacist to show you.
Is it okay to mix liquid medicine with juice or food?
Only if the pharmacist says so. Some medicines lose effectiveness when mixed. Others can change how they’re absorbed. Always ask before mixing. If you’re told it’s okay, still measure the full dose first, then mix it. Never pour medicine into a full cup of juice and assume the whole cup is the dose.
Why do some labels still have "tsp" on them?
They shouldn’t. Since 2016, the FDA has required all new prescriptions to use only mL. If you see "tsp," it’s likely an old label from a pharmacy that hasn’t updated its system. Report it. Ask for a new label with mL only. You have the right to a safe, standardized label.
13 Comments
Write a comment
More Articles

Top Alternatives to FelixForYou.ca for Telemedicine in 2025
Discover the leading alternatives to FelixForYou.ca, a Canadian telemedicine platform, focusing on digital healthcare options available in 2025. Highlighting Maple Health, Tia Health, Livewell, Telus Health, and Jill Health, this article provides insights into each service's offerings, pros, and cons. Whether looking for 24/7 access to healthcare professionals, adaptable programs, or specialized medical services, these alternatives cater to varied health needs. Consider factors such as accessibility, cost, and service range to choose the right telemedicine solution.

Prepaid Drug Mail-Back Envelopes for Medication Disposal: How They Work and Where to Get Them
Prepaid drug mail-back envelopes let you safely dispose of expired or unused medications by mail-no trips to a pharmacy needed. Learn how they work, what you can send, and where to get them for free.
Minoxidilfinasteride and Hair Loss in Travel: Tips for Staying Confident on the Go
Traveling can be stressful, especially when dealing with hair loss. Thankfully, Minoxidilfinasteride has been a game changer in managing this issue. To stay confident on the go, I make sure to stick to my treatment routine and pack my Minoxidilfinasteride in my travel kit. I also carry a hat or a stylish scarf to cover up any thinning spots. Most importantly, I remind myself that confidence comes from within, and I don't let hair loss hold me back from enjoying my travels.
phyllis bourassa
March 6, 2026 AT 12:58Oh honey, I’ve been there. Stared at that label like it was ancient hieroglyphics. My kid had a 0.8 mL dose and I used a spoon because I was tired. Ended up in the ER at 2 a.m. with a panicked toddler. Don’t be like me. Just get the damn syringe. They give them for free. Seriously. Ask. Again. And again. Your child’s life isn’t a guessing game.