
Why Returning to Work Doesn't Have to Mean Suffering
If you have chronic pain, the thought of stepping back into an office environment can feel overwhelming. You might worry that your boss won't understand why you're moving slowly or needing extra breaks. That fear is real, but you are not alone. Current estimates suggest that roughly 51.6 million adults in the U.S. experience chronic pain, yet most manage to hold down jobs with the right support.
Chronic Pain is defined as persistent pain lasting longer than three months. It significantly impacts daily life, often limiting major activities like walking, lifting, or sitting for long periods. Under legal frameworks like the Americans with Disabilities Act (ADA), this condition qualifies as a disability when it substantially limits these activities. Knowing this distinction matters because it unlocks specific rights you may not know you have.Understanding Your Workplace Rights and Protections
Many employees hesitate to ask for help because they assume accommodations cost a fortune. In reality, the Job Accommodation Network reports that 56% of accommodations cost employers nothing to implement. For those that do have a price tag, the median one-time cost is surprisingly low at around $300. Understanding the landscape of employment law helps demystify the process.
The Family and Medical Leave Act (FMLA) provides up to 12 weeks of unpaid, job-protected leave annually for eligible employees. While this offers breathing room during acute flare-ups, it does not guarantee the daily modifications needed for a permanent return. That protection comes from the Rehabilitation Act of 1973 and the ADA, which cover federal agencies and private sector employers with 15 or more employees respectively. These laws require an interactive process where both parties discuss what works.
Types of Accommodations That Actually Help
When planning a return, vague requests lead to confusion. Successful plans hinge on specificity. Instead of saying "I have back pain," you say "I need a sit-stand desk and 10-minute movement breaks every 90 minutes." Below are the most effective categories of modifications backed by clinical data.
| Type | Examples | Estimated Cost |
|---|---|---|
| Physical Adjustments | Adjustable standing desks ($300-$1,200), specialized keyboards ($50-$300), footrests ($25-$150) | $50 to $1,200 |
| Time-Based Changes | Flexible start/end times, additional breaks (5-15 mins every 1-2 hours) | None |
| Environmental Modifcations | Temperature control adjustments, relocating workspace closer to restrooms | None to Low |
| Assistive Technology | Voice recognition software ($100-$300), heated cushions ($50-$200) | $50 to $300 |
Research indicates that physical adjustments like ergonomic chairs and standing desks reduce fatigue significantly. For conditions involving heat sensitivity, such as multiple sclerosis, temperature control systems become critical. Environmental factors matter too; relocating a workstation to minimize walking distances can prevent exhaustion for someone who gets fatigued after walking 200 feet. These changes aren't just luxuries; they enable functional performance.

Navigating the Interactive Process Successfully
The most critical step is documentation. You need medical records specifying the diagnosis, functional limitations, and specific recommended accommodations. Dr. Wong's research found that case-by-case accommodations resulted in a 78% job retention rate compared to 42% for generic solutions. Generic statements like "I need pain relief" are often denied. Specific requests like "I need a heated massage cushion costing $85 that plugs into standard outlets" yield higher success rates.
Engaging in good faith dialogue is required by law. Employers cannot force you to accept a specific accommodation, but they must work with you to find one that solves the limitation. Federal agencies typically respond within 10 business days, while private sectors must respond promptly though timelines vary. If you hit a wall, resources exist to mediate. The Job Accommodation Network resolves 82% of inquiries without formal complaints. Utilizing Occupational Therapists is another strategy; their assessments identifying ergonomic adjustments have been shown to reduce work limitations by 37%.
Overcoming Fear of Discrimination
Data shows that 62% of employees with chronic pain delay requesting help due to fear of discrimination. About 31% end up leaving their jobs rather than disclosing their condition. This fear often stems from a lack of clear precedent. Supervisor attitudes play a massive role here. When coworkers and managers support the plan, retention improves drastically.
Successful implementation relies heavily on clarity. Federal employee reports indicate that clear specifications result in an 89% approval rate versus 45% for vague requests. Documenting how symptoms affect functions is your shield against denial. For example, if you need flexible scheduling to attend physical therapy appointments, state exactly how much time is needed and how the work output remains consistent despite the shifted hours.

Addressing Common Challenges and Denials
Sometimes requests get turned down. A significant portion of denials happens because employers misunderstand that accommodations can be temporary during flare-ups. Some assume the fix needs to be permanent forever. Clarify that the plan can evolve. Another hurdle is the concept of "undue hardship." This means the accommodation creates significant difficulty or expense relative to company size. Small businesses might face higher hurdles than large corporations, but the threshold for "undue hardship" is quite high legally.
Long-term trends show a growing acceptance of graduated return-to-work approaches. Employees returning at reduced hours (20-50% of normal) initially see 63% higher retention than those jumping straight into full-time roles. Additionally, long COVID-related chronic pain is increasingly recognized under disability protections, broadening who qualifies for these plans. As wearable technology becomes more common, objective documentation of functional limitations might replace some subjective reporting, currently used in about 7% of cases.
What proof do I need to request accommodations?
You generally need medical documentation that specifies the diagnosis, outlines your functional limitations, and recommends specific accommodations. Vague notes are insufficient; the document should clearly link the medical condition to the workplace need.
Can my employer refuse an accommodation?
Employers can refuse if they can demonstrate 'undue hardship,' meaning significant difficulty or expense relative to the company's size and resources. However, they cannot simply reject it without offering an alternative effective solution.
Are accommodations always permanent?
No. Accommodations can be temporary during flare-ups or recovery phases. Graduated return plans often involve reduced hours that increase over time as your health stabilizes.
Does the ADA protect everyone?
The ADA applies to employers with 15 or more employees. State laws like California's Fair Employment and Housing Act may extend this to smaller firms with 5+ employees.
How much does an accommodation cost?
Most cost nothing. Of those with costs, the median one-time expense is around $300. Examples include ergonomic chairs, voice recognition software, or footrests.
Next Steps for Your Plan
Start by gathering your medical records. Write down exactly how your pain stops you from performing specific tasks. Reach out to HR with written documentation referencing the relevant disability guidance. Consider bringing in an Occupational Therapist to assess your workspace. Remember, nearly half of all employers find ways to accommodate without financial strain. Your goal is sustainable employment, not perfection. Communicate early, be specific, and track your progress. If issues arise, knowing the difference between a legal violation and a budgetary hurdle will help you negotiate effectively.
15 Comments
Write a comment
More Articles
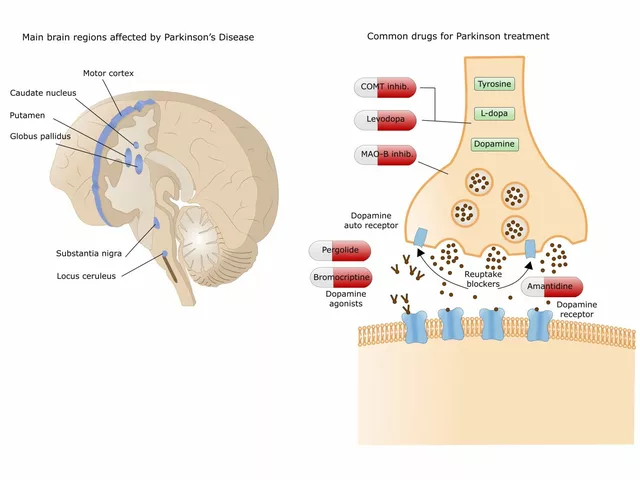
The potential benefits of betahistine for individuals with Parkinson's disease
In my recent exploration, I discovered the potential benefits of Betahistine for those living with Parkinson's disease. This medication, often used for vertigo, could potentially improve symptoms of this neurodegenerative condition. Researchers suggest that Betahistine might have the ability to reduce tremors and improve motor function. There is also a belief that it could enhance cognitive abilities and alleviate depression often associated with Parkinson's disease. However, it's important to note that more research is needed to confirm these potential benefits.

Poison Control Hotline: How It Works and What to Report About Medications
Learn how the poison control hotline works, what details to report about medications, and why calling 1-800-222-1222 can prevent ER visits and save lives. Free, expert help 24/7.

Telehealth Strategies for Monitoring Side Effects in Rural and Remote Patients
Telehealth is transforming how rural and remote patients manage medication side effects. From smart devices to pharmacist-led monitoring, discover how these strategies reduce hospitalizations and save lives in underserved areas.
Victor Ortiz
April 1, 2026 AT 15:17The statistical probability suggests compliance is low regardless of legislation claims. Companies operate on profit margins that rarely account for disability costs. The data presented assumes good faith negotiations which is a naive position to hold. Employers prioritize continuity of operations over individual health outcomes consistently. Legal frameworks exist but enforcement mechanisms remain incredibly weak in practice.